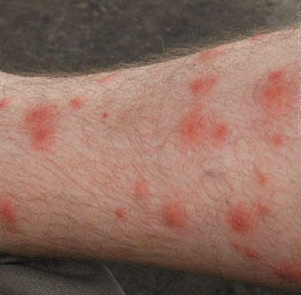
See your GP or pharmacist if you think your child has impetigo. Non-bullous impetigo typically affects the skin around the nose and mouth, causing sores that quickly burst to leave a yellow-brown crust.īullous impetigo typically affects the trunk (the area of the body between the waist and neck), and causes fluid-filled blisters that burst after a few days to leave a yellow crust. There are two types of impetigo called non-bullous and bullous. It isn't usually serious and often improves within a week of treatment. Impetigo is a common and highly contagious skin infection that causes sores and blisters. Make sure your child drinks plenty of fluid, and if eating and swallowing is uncomfortable, give them soft foods, such as mashed potatoes, yoghurt and soup. Your child's immune system will fight the virus and it should clear up after about seven to 10 days. There's no cure for hand, foot and mouth disease and it's easily spread, so you should keep your child away from school or nursery until they're better. It's most common in young children (particularly those under 10), but it can also affect older children and adults. Hand, foot and mouth disease is a common, contagious infection that causes mouth ulcers and spots and blisters on the palms of the hands and soles of the feet. This more severe form is called Stevens-Johnson syndrome and it can be life-threatening. In rare cases, erythema multiforme can be triggered by a reaction to certain medications, such as an antibiotic or anticonvulsant. It may take from two to six weeks before they feel better. See your GP if your child has a rash and seems unwell. Your child will probably feel unwell and may have a fever, which you should be able to treat with over-the-counter medicine. The hands or feet tend to be affected first, followed by the limbs, upper body and face. The spots look like targets, with a dark red centre and paler ring around the outside. Erythema multiformeĮrythema multiforme is a skin rash (usually mild) that's caused by an allergic reaction to the herpes simplex virus. It isn't a serious condition, but if your child later becomes infected with the herpes simplex virus, it can cause the eczema to flare up into an outbreak of tiny blisters called eczema herpeticum, and will cause a fever.Ībout one in five children in the UK has eczema, and in eight out 10 cases it develops before the age of five, often before a child's first birthday. The most common type is atopic eczema, which mainly affects children but can continue into adulthood.Ītopic eczema commonly develops behind the knees or on the elbows, neck, eyes and ears. EczemaĮczema is a long-term condition that causes the skin to become itchy, red, dry and cracked. For example, paracetamol can help relieve fever (don't give aspirin to children under 16), and calamine lotion and cooling gels can be used to ease itching. There's no specific treatment for chickenpox, but you can take steps to relieve the symptoms. Some children only have a few spots, whereas others have them over their entire body. The spots are most likely to appear on the face, ears and scalp, under the arms, on the chest and belly, and on the arms and legs. It most commonly affects children under 10 years of age.Ī rash of itchy spots turns into fluid-filled blisters. They crust over to form scabs, which after a while drop off. ChickenpoxĬhickenpox is a viral illness that most children catch at some point. It usually responds well to treatment with antibiotics. If you can't see your GP on the same day, go to a walk-in centre or minor injuries unit.Ĭellulitis can usually be diagnosed by assessing the symptoms and examining the skin. See your GP immediately if an area of your child's skin suddenly turns red, hot and tender. Your child will probably also have a fever. It often affects the legs, but can occur anywhere on the body. The affected area will be red, painful, swollen and hot. CellulitisĬellulitis is an infection of the deeper layers of skin and underlying tissue. The most common causes of rashes in children are:Īlthough meningitis has become less common over recent years, it's important to be aware of the rash and the other signs and symptoms of meningitis. This page may give you a better idea about what could be causing the rash, but don't use this to self-diagnose your child's condition – always see a GP for a proper diagnosis. They'll be able to investigate the cause and recommend any necessary treatment. However, see your GP if your child has a rash and seems unwell, or if you're worried. Most rashes are harmless and disappear without the need for treatment. Childhood rashes are common and aren't usually a cause for concern.
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
